Chapter Five
Body Parts
Ears
I didn't know
I had psoriasis in my ears until one derm discovered
it. “Oh boy, you got it here, too.” That meant yet
another prescription — a liquid steroid solution —
and the need to start ensuring a supply of Q‑tips™.
For many
months thereafter the ear psoriasis remained deep in
my ear canals and I had to leave my solution and
Q‑tips™ in sight or I'd forget the twice daily
applications. But eventually this manifestation
decided to grow, too. It crept slowly out of my ear
canals and spread over the folds of my outer ear.
Then it became more symptomatic of the psoriasis I
knew and hated; i.e., itching, flaking visibly, a
more or less constant irritant.
I do what I
can to keep my outer ears flake free, but I believe
what I'm told: remove flakes by picking at them when
the lesions are dry and you're more than likely to
compound the problem as well as bleed. So, I've
tried to avoid getting into the habit of picking at
my ears, especially in public, and to mask the
psoriasis I've let my hair grow longer.
The ear
psoriasis has come in handy. My second wife used to
chastise me for “not listening to her” when she was
trying to irritate me.
“You don't
hear a word I say.”
“Well, honey,
it must be the psoriasis, see?” Then I'd show her
and for a few days she'd leave me alone.
Hands
My hands
erupted on an extended business trip to Washington,
DC and several points in Ohio, in mid 1995. I have
plaque psoriasis on the backs of my hands and
pustular psoriasis on the palms of my hands. The
only effective therapy has been high potency steroid
cream and wearing so called “food handlers' gloves”
overnight. I ran out of high potency steroid cream
on this business trip, and had no food handlers'
gloves with me. My hands had been quiet for weeks
before this trip, so I stupidly wasn't worried.
About ten days into the trip I looked like a leper.
For me, hand
psoriasis is the worst. You can't hide it (short of
wearing gloves, which is equally conspicuous), it's
tremendously uncomfortable (itching, cracking and
soreness), and it can be debilitating to someone
whose work involves a lot of typing.
My trip to
Ohio was a corporate television field production
expedition. The producer/videographer and I (her
assistant) visited a factory in Cincinnati to shoot
two days of video “on location.” En route from DC to
Cincinnati, we stopped over night at the producer's
parents' home in a small Ohio hamlet north of
Columbus. My hands looked like they'd been dipped in
acid or held over an open flame. I felt like Freddy
Kruger. As is usually the case, people couldn't help
but notice then felt embarrassed about staring and
unwilling to ask probing questions. But, also as
usual, innocence overcame inhibition and a four-year-old finally broke the ice.
We were
sitting on the patio on a humid afternoon. I was
doing my best to conceal my condition by hiding my
hands between my crossed legs, but I'd been served a
beer and this meant I had to occasionally grasp the
can. Little Jacob saw my hand while I took a sip,
charged up to me and said, loud enough for all to
hear, “Ouch?”
What could I
do? I let little Jacob peruse my hand and said,
“Yes, ouch.” This caused a momentary embarrassing
pause in the adults' conversation, but they
recovered quickly. At least I was less timid as I
finished my beer.
Two days after
the little-Jacob episode, I was with my producer
on location in Cincinnati. She was picking and
setting up shots. I was dragging equipment around
and, supposedly, getting people ready to be
interviewed. This meant attaching their lavaliere
microphones to their clothes and getting them
comfortably seated for the interview. Only none of
them were too comfortable having someone whose hands
looked leprous run microphone cable under their
jackets and apply powder to their foreheads. The
women interviewees seemed especially fearful.
When you're on
a field shoot in someone else's back yard, you don't
like to make waves, so I cast desperate glances to
the producer/videographer. Eventually she relented,
did her own miking and powder jobs. Nobody after
that had to be exposed to my “disease.” I carried
cables and equipment around twice as hard, logged
shots (i.e., wrote down where she pointed her
camera), and just tried to be relevant and
necessary.
Fingernails
I'd read about
nail psoriasis long before I ever manifested it, so
when it finally happened at least I knew what was
going on. The gross deformation of the nails caused
by psoriasis can be socially paralyzing — you just
can't hide the tips of your fingers all the time!
I'm told some
people have their psoriatic nails removed and
replaced with artificial nails but, when the
psoriasis manifests under the nail bed, won't such a
procedure be a short fix at best? I don't know; that
level of vanity is not my problem.
In fact, when
I was a boy a manicurist told me my nails were
“hopeless,” and that was years before psoriasis and
I made our tryst. The manicurist worked at the
barbershop where I shined shoes. The proprietor of
the shop was particular about his bootblacking. “You
put the wax on your bare hands and you rub it into
the shoe with your skin — your leather to the shoe's
leather.”
The
manicurist, a pudgy middle aged woman with no
disposition whatsoever, thought this was an assault
on personal hygiene. Often, when the shop was empty,
she'd call me over to her station and labor to get
the shoe wax out from under my nails. It was during
one such session that she said my nails were
“hopeless.”
She based that
prognosis on the ragged evidence that I was an
accomplished nail biter. I'd be the first to admit:
psoriasis or no, you'd not want my hands to appear
in close-up on your TV commercial.
 Nonetheless,
watching the nail psoriasis hit both my thumbs at
the same time was a real horror show. In many
respects nail psoriasis can be the most insidious
variety because it manifests slowly and acquiesces
even slower. In my case, the psoriasis in the
thumbnails first appeared as a yellowing of the
“moons” just beyond the cuticle. Then the “yellow”
part of the emerging nail pushed up so the nail had
a distinctive ridge. Over the next weeks and months
the nail grew like an ugly yellow wave, up and down.
Eventually, the nail was totally corrupt, from
cuticle to the end I chewed off. I really did look
like something a horror movie special effects
supervisor would love to replicate.
Nonetheless,
watching the nail psoriasis hit both my thumbs at
the same time was a real horror show. In many
respects nail psoriasis can be the most insidious
variety because it manifests slowly and acquiesces
even slower. In my case, the psoriasis in the
thumbnails first appeared as a yellowing of the
“moons” just beyond the cuticle. Then the “yellow”
part of the emerging nail pushed up so the nail had
a distinctive ridge. Over the next weeks and months
the nail grew like an ugly yellow wave, up and down.
Eventually, the nail was totally corrupt, from
cuticle to the end I chewed off. I really did look
like something a horror movie special effects
supervisor would love to replicate.
No derm has
been able to offer an effective topical remedy for
my psoriatic nails. One fellow talked me into
something called “Russian Formula.” This was an
unguent comprised of beeswax and something really
nasty. It was applied liberally to my right thumb
nail. Then they covered it with plastic (occlusion)
and then standard medical gauze and tape. My
instruction was to keep all this dry and in place
for ten days. What happens after ten days? I asked.
I was told my nail would peel off allowing a new
nail, hopefully a healthy nail, to grow back in
time. Meanwhile I would just walk around without a
thumbnail.
Sounds a
little radical to me now, as I write this, but I do
recollect how grotesque the psoriatic nail looked,
and how anything, even having no nail
whatsoever, sounded better at the time.
Well, trying
to keep your thumb dry for ten days is easier said
than done. I showered with a latex glove on that
hand; tried unsuccessfully to keep the dressing
clean.
The night
before I was scheduled to have the dressing — and
nail — removed, Lexington got hit with one of its
worst snow storms in years. I made it to the
dermatology clinic but the good doctor who'd
administered the “Russian Formula” did not. But it
was okay; another derm was there and volunteered to
fill in.
Off came the
dressing — what a relief! There was the nail,
psoriatic, ugly and a bit rubbery. It wouldn't come
off. The stand-in derm even went at it with a
scalpel and managed to cut my nail bed severely.
As it ended, I
drove home over icy streets with a new dressing on
my thumb, this one to prevent infection. The nail
had survived, was still there. As I was checking out
of the doctor’s office, I said to the cashier, “Next
time I'm going to try Scandinavian Formula.” She
smiled and nodded and hadn't the foggiest idea what
I was talking about.
When nail
psoriasis spread beyond my thumbnails to,
eventually, affect every nail on both hands, I got
desperate. At the time I was developing some
computer software applications for a client of mine
and I was expected to demonstrate the software for
the office staff. That meant sitting at a keyboard,
office workers hovering around me, while I typed and
described the elegance of my handiwork.
The
inelegance of my hands themselves made me
extremely self conscious.
The night
before the grand demo I went at my deformed nails
with an emery board and much to my surprise (or
maybe I was fooling myself) I seemed to achieve some
improvement in their appearance. I managed to level
out some of the ridges, straighten up some of the
rough edges. Yeah, anybody who took a look would
know something was grossly wrong here, but the nails
weren't as bad as they had been prior to the emery
board treatment.
Later, I got
real creative. I rigged a way to attach
sandpaper to an electric screwdriver. Talk about
your high tech manicure! My fingertips were
literally smoking.
Because I'm
nuts or something, that year I concluded the family
holiday video to my parents with a macro‑close-up of
my nail psoriasis and a narrative description of the
way I was “sanding off the rough spots.” My dad took
this to heart and bought me a high speed handheld
router for Christmas, complete with a set of sanding
tips.
I've since
cooled to this method of cosmetic dermatology for
nail psoriasis — especially after the pinky finger
on my left hand caught fire.
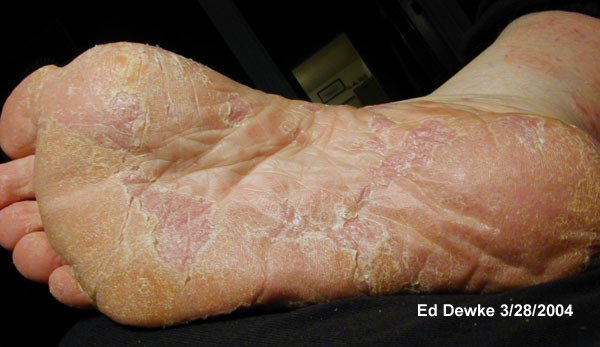
Feet
I remember
saying to myself, when my hand and nail psoriasis
was first getting bad, “Why couldn't it be my feet?”
The psoriasis gremlin eventually answered: “Why not
your hands and your feet?”
I'm fortunate
in that I can stay more or less gainfully employed
and not spend a lot of time on my feet,
because when the plaque psoriasis rages on your
feet, walking can be painful.
My office is
in my home. Yes, I'm one of those lucky stiffs who
can leave their ties in the closet on most days and
spend weeks in those old, stretched out, comfortable
loafers or athletic shoes. But I own a few pairs of
nice dress shoes just like I own a few suits — for
funerals, weddings and equally morbid business
appointments.
There are a
few cities in which I really love to have overnight
business, because such trips give me an opportunity
to enjoy these cities. New York is one of these.
When I'm in Manhattan I walk. Doesn't everybody? I
walk to lunch, dinner, shows; I walk along the
waterfront.
One of my
favorite Manhattan walks is from Times Square down
to South Ferry. I love to arrive at South Ferry just
after nightfall, then take a round-trip on the
Staten Island Ferry to enjoy that illuminated New
York skyline as we chug past Liberty Island.
On one such
trip to Manhattan in the spring of 1994, I decided
to take my late afternoon midtown‑to‑downtown walk
and did so, because I had no alternative, in my
business attire. This included a crisp pair of tight
Oxfords which, though several years old, hadn't seen
but a few blocks of wear. They still weren't really
“broken in.”
 My feet were
“beginning to holler” by the time I got to South
Ferry, but I blamed this on the shoes. I'm sure it
had a lot to do with the shoes.
My feet were
“beginning to holler” by the time I got to South
Ferry, but I blamed this on the shoes. I'm sure it
had a lot to do with the shoes.
I remember
sitting in my hotel room later that night, watching
TV and quite casually rubbing my “sore” feet. That
night I didn't pay much attention to what else
might be wrong with them.
I had another
business appointment the next day and noticed before
my shoes had been on for an hour that my feet were
really hurting. “I just over did it with my walk
yesterday,” I said to myself, and tried to make it
through the meeting, then lunch, then the next
meeting without limping visibly.
After my last
meeting of the day, I relented and took a cab back
to the hotel.
That evening I
noticed the big red splotches running down the sides
of my feet, and the scattering of nickel sized
lesions on the instep. “Welts,” I thought. Those
shoes were just too damned tight to walk in.
I didn't
really suspect psoriasis until I was back home, back
in my comfortable athletic shoes, but still limping
around. When I took my next close look the real
culprit became clear. Those red “welts” were
flaking. It was most prominent after I spent several
hours barefoot. I rather imagine that's because my
feet had an opportunity to dry out, hence the extra
thick layers of psoriatic dermis at the surface
turned white and scaly, just like on every other
plaque lesion.
I've learned
the foot lesions aren't particularly difficult to
treat — especially those on the insteps — if you
wear loose shoes. I've been more or less successful
with high potency steroid ointments. Thick lesions
on the soles of the feet are more problematic; for
one, like corns, walking on them can put pressure on
the nerves beneath — hence the pain. Also, I think
the very act of standing and walking on these
lesions has much the same effect scratching other
lesions has: it irritates them, magnifying the
condition.
The next time
I was on a business trip in one of my “walking
towns” and didn't have comfortable shoes to change
into, I smartened up. The first thing I did was walk
to a department store to buy some comfortable
shoes.
The lesions on
my feet are ever present; they wax and wane like all
the others. I've read or been told that occlusion
therapy can work on feet just like it works on
hands; however, I've not heard of “food handler's
slippers” that work like “food handler's gloves.”
I've thought about going to bed with large size
freezer bags over my feet and taped to my ankles,
but gosh, what if my house caught fire and I had to
run outside and be seen by my neighbors? What would
they think of me in my shower cap, wearing a pair of
food handler's gloves on my hands, and sporting two
freezer bags on my feet?
Privates
If you just
sat there and got psoriasis, and didn't move, and
didn't aggravate the lesions, you would probably
live until you starved. Skin growing fourteen times
faster than normal is not typically fatal (for
humans). Ironically, derms seem more concerned about
the consequences of treating psoriasis than they do
about the disease itself (as well they should given
the nasty side effects of some of the treatment
regimens). The exception to this is any and all
psoriasis activity that “breaks” the skin. When you
bend skin that is overly thick (or overly thin) and
overly dry it will tend to crack; and when this
happens it's just like having a cut or a scratch —
infection can set it. Infection is a threat when the
skin breaks or cracks, but usually before infection
becomes a problem there's the pain with which to
contend. When psoriasis hurts — I mean, really
hurts — it's often because the affected skin has
cracked.
At one time or
another, I have had this happen to most of my
lesions. That's because I, like every other
psoriatic, am not at leisure to just sit there and
manifest the disease. I, like every other psoriatic,
have to get up and move around — get on with life.
Here is something I learned the hard way: The skin
over your joints isn't necessarily that which has to
be most “flexible.” There are a couple of other
areas where skin elasticity is very important — your
anus and your genitals.
All right, now
you know what I'm about to get into is unpleasant.
I'll definitely understand if you want to skip this
part.
In the Fall of
1993 I was working on an extended assignment in
Washington, DC, when I learned I was needed for one
day in Philadelphia. Normally, you'd hop a train to
commute from DC to Philly and back, but I decided to
rent a car and drive back through Lancaster County,
Pennsylvania — a part of the country I really love
and hadn't visited for nearly a decade. On the
outbound part of that drive my anus began to burn.
It literally felt like someone was holding a lit
match under my seat. I'd never felt pain quite like
this before.
As I cruised
along sweating profusely, I tried to determine what
the matter was. Because I had no history of such a
sensation, all that I could conjure was images of my
father, thirty years earlier, when he was suffering
from hemorrhoids. The pain used to make him sweat,
too.
I managed to
get through my appointment in Philadelphia and
start the motor trip back, but I couldn't make it
all the way; it was just too damned painful to sit
and drive. At least I had the tenacity to make it to
Lancaster County, where I found a motel and looked
forward to a good soak in the tub. While the tub was
filling I used the commode...
...and
thought that I would not live to see another Sunday!
I look back on
the experience now and call it “The Agony of
Evacuation.” I don't want to go into further detail;
just remembering it still makes me sweat.
I just knew it
was hemorrhoids and made an appointment with my GP
long‑distance to ensure he could see me the
minute I got back home to Lexington, Kentucky.
“Who is your
dermatologist?” my GP asked while he was conducting
his “behind‑my‑back” examination.
I told him.
“Has he
examined this?”
“Examined
what? My butt?”
It wasn't
hemorrhoids, it was a psoriatic lesion “involving”
the anus, and it had cracked (no pun intended).
My GP and my
derm put their heads together and came up with
yet another expensive topical unguent — a
moderately potent steroid cream combined with an
antibiotic. Thank God, it worked
Now, flip me
over. Psoriasis on the genitals. That's another
story.
I can only
address my own experience with psoriasis on the
penis. I've no personal, anecdotal or clinical
experience with psoriasis on the vulva (but my heart
bleeds for those who do).
“Damn! It
hurts,” I said and reluctantly rolled away. The room
was dark.
“Is it me?”
she asked, tenderly.
Snap. A lamp
went on. I was blinking while my eyes adjusted to
the light. “Oh Lord!” she exclaimed, “You're
bleeding!” Sure enough, I was.
Forget my
pain. How do you suppose that made her feel?
Upon
examination the problem was obvious. A quarter sized
lesion on the inner side of the penis, encompassing
the foreskin, had stretched beyond the limit of its
psoriatic durability and cracked during intercourse.
Until that moment I hadn't known I had this lesion.
(Rather wish I still didn't know, to be
honest with you.)
Here again derms
go gentle with the steroid creams. I was prescribed one
of the mildest on the market; but I didn't let my derm
off the hook so easy.
“So,” I said,
“Maybe this stuff will quiet it down, maybe it won't ...
but if it's like every other lesion on my skin, we know
it won't go away forever. Is it not safe to have sex if
this lesion is flaming?”
“Use a lubricant,”
he said. “And be gentle.”
I'm just glad the
solution wasn't occlusion therapy.
●●●●●
Ed’s Postscript (2/20/2008):
My ears have continued to flake,
on and off, even after I started systemic therapies.
Flaking ears plagued my father his entire life, but it
wasn’t diagnosed as psoriasis until he was in his late
sixties or seventies. As far as I know, the ears were
the only place he ever did
flake. Eventually my derm and I discovered Fluocinonide
solution was best at subduing psoriasis activity both
outside and inside my ears. As with most topical
corticosteroids in my experience, the Fluocinonide
solution works best if it is used sparingly and
infrequently.
Occlusion continued to be the only answer
for my hand psoriasis until I started taking systemic
meds. And occlusion was only reliable with potent
corticosteroid ointments like clobetasol or
betamethasone. But occlusion never did much for my nail
psoriasis. The first treatment I had that eradicated
nail psoriasis long enough
for healthy nails to replace the corrupt ones was
cyclosporine, an oral systemic used primarily to dampen
tissue rejection in transplanted organ recipients.
Flakers take much smaller quantities than transplant
patients, so we can usually remain on the medicine for
longer. High blood pressure, fluid retention leading to
edema (swelling) and kidney dysfunction are the side
effects that usually signaled me to stop my course of
cyclosporine — and that usually had to happen after 10
months on the drug. I was also lucky about my
cyclosporine rebounds (return of psoriasis when the drug
is stopped). Skin lesions would return relatively
quickly with the exceptions of hands, feet and nails.
All of these parts stayed clear longer than the rest of
me.
The fact that
cyclo helped my nails while occlusion did not may have
something to do with where it started. For nail
psoriasis, lesion activity can be in the nail matrix,
where the cellular activity that generates new nail
material occurs. This is beneath and further down the
digit from the cuticle and “moon” of the nail. If the
psoriasis dysfunction is causing tissue growth in the
nail matrix to occur too fast, the ridges and thickened
nails will happen. But lesion-like activity can also
happen directly beneath the nail, in the nail bed. In
this case, scale similar to what we experience on other
skin lesions builds up beneath the nail, lifting it and,
sometimes, causing it to separate completely from the
finger. When my nail psoriasis was at its worst, the
skin on top of my cuticle was always inflamed. To me
this suggested the underlying nail matrix was the
culprit.
It’s been true
for me that once I’ve had a significant lesion, that
place on me doesn’t forget and future lesions are likely
to occur right there, too. My anus has been no
exception. Fortunately, now I know when it’s starting to
happen. Fast use of the corticosteroid/antibiotic cream
thwarts the problem before it gets to the awful stage I
reached on my painful journey to Philadelphia all those
years ago.
Genital psoriasis is among my most
recalcitrant types. I get
inverse psoriasis, which is a
type characterized as inflamed but without flakes and
thickening. At times it virtually engulfs my scrotum,
parts of my penis, and the folds of skin that attach all
of this to my groin. In 2003 I had an
orchiectomy
(removal of a cancerous testicle). My genital P was
active at the time and I anticipated a Koebner
Phenomenon response to the surgery that would make it
even worse. Well, it didn’t get worse, but since that
time it has been ever-present. When my genital inverse
psoriasis is flaring it itches terribly, but giving it a
good scratch (when occasion permits) is an awful
idea. It seems to take a lot of scratching to make the
itch subside and then, over the next quarter of an hour
or so, what you scratched catches fire. Literally. Like
somebody is holding a lit match to your balls (or, in my
case, “ball”). So, it should come as no surprise that,
in the Dewke household, anti-itch cream is ALWAYS at
hand.